SingaporeMotherhood | Baby & Toddler
April 2018
6 Most Common Reasons Why Children in Singapore End up in the A&E

As many as 500 children in Singapore are seen at the A&E (Accident and Emergency) department on average every day. These are the most common reasons why.
According to Dr Jade Kua, Consultant, Department of Emergency Medicine at KK Women’s and Children’s Hospital, true emergencies made up about two per cent of the total attendance to KKH’s Children’s Emergency in 2017. True emergencies are those that require immediate medical attention, such as those who were in serious road traffic accidents resulting in multiple organ damage or those with severe asthma attacks with low oxygen levels.
[banner][/banner]
“We also have a category of urgent cases who are triaged to be seen early, such as newborn babies or children in pain, or stable children with fractures and open wounds. Such urgent cases made up about 53 per cent of the total Children’s Emergency attendances last year,” adds Dr Kua.
Just about every parent has experienced this nightmare: It’s the middle of the night and your kid is really unwell. Should you wait till the morning to see a GP or rush them to the hospital immediately? Below is a list of common reasons parents take their children to the A&E. How do we know when it’s truly an emergency? Apart from using a mother’s intuition, this guide should help you decide.
1. Acute Diarrhoea / Vomiting

“It was about 2am when I rushed Oliver to the A&E at KKH because he had projectile vomit that was bloody,” shares 33-year-old public service officer Chong Poh Choo. “Because the A&E doctors initially didn’t know where the blood was coming from, we were escalated to emergency status, which was really scary.” As it turns out, the diagnosis was stomach flu and the forcefulness of the vomit was what had caused his oesophagus to bruise and bleed. Thankfully, 20-month-old Oliver recovered well after staying in the hospital for five nights.
All of us have suffered throwing up, loose stools and tummy pains from gastroenteritis (an infection of the intestinal tract) at some point in our lives. However, in babies and young children, prolonged diarrhoea and vomiting can result in serious dehydration if left unchecked. The leading cause is exposure to viruses, either through contact with an infected person, touching contaminated items or surfaces, or consuming contaminated food or drink. A common culprit is rotavirus, the cause for about 40 per cent of children who are hospitalised due to gastroenteritis.
Go to the A&E if there is persistent and severe abdominal pain or fever, bloody stools, bloody or green vomit, signs of dehydration (eg. dry tongue and lips, acting lethargic, decreased or no urine for six hours).
(See also: Baby’s Crying and Vomiting Non-stop. Could it be Intussusception?)
2. Breathing Difficulties

“Elliott ended up in hospital two weeks before his second birthday. He had been coughing and wheezing. That day, he refused all food and had trouble falling asleep. I decided to bring him to the hospital to be nebulised so that he could have a good night’s sleep,” relates Monica Eng, 40, stay-at-home mum. The doctors at the KKH A&E diagnosed Elliott with acute bronchitis. Apart from wheezing, he had to stay in hospital due to low blood oxygen levels that required oxygen supplementation. The doctors only discharged Elliott a week later, when his blood oxygen level was back on track.
When children suffer from upper respiratory tract infections such as bronchiolitis and sinusitis, breathing may be compromised. What starts as a simple cold may lead to severe coughing, wheezing, breathlessness and fever. Left unchecked, the infection may worsen and pneumonia may set in. If your child suffers from asthma, a trigger may cause sensitive airways to narrow and cause breathing difficulties. Ensure that your doctor-prescribed inhalers are always on hand in case of an asthma attack.
Go to the A&E if there is increased laboured breathing, pale or greyish skin colour (hurry!), difficulty sleeping, feeding or drinking, is lethargic, has a persistent high fever. In an acute asthma attack, if your child is having a more severe attack than usual, is not responding to usual medication, requires an inhaler more than once in four hours, is tiring from the effort of breathing or not fully alert (hurry!).
(See also: When Your Child is in Hospital)
3. High Fever

Dawn Hoh, 41, is a cool stay-at-home mum of three who doesn’t like to overreact. “Lorraine had a raging fever for two weeks at 22 months old. She was also having full-blown flu symptoms, having not even had so much as a sniffle up till then. My husband was afraid it might be intestinal intussusception, so we finally took her to the A&E.” A few hours later, Lorraine was discharged after undergoing a scan that ruled out the ‘telescoping’ intestinal issue. “The doctors prescribed medication to help bring her temperature down and she soon recovered,” added Dawn.
It’s important to understand that a fever is not an illness, but rather a symptom of an infection. While it’s hard to remain calm when your little one’s temperature rises, a high fever (38.5°C and above) doesn’t automatically mean it’s critical. Similarly, writing off a low-grade fever as a small matter may be unwise too. So how do we know when to start panicking? Well, instead of just going by the numbers on a thermometer, look for other signs. For instance, is your child still playing and eating well? If so, you may give them Paracetamol syrup – making sure it’s the correct dosage – and adopt a wait-and-see approach.
Go to the A&E if the fever is accompanied by breathing difficulties, signs of dehydration, severe stomach discomfort and vomiting, rash, lethargy, or if your baby is under three months old and has a fever.
(See also: What to Do If Your Child’s School Has an HFMD Outbreak)
4. Convulsions
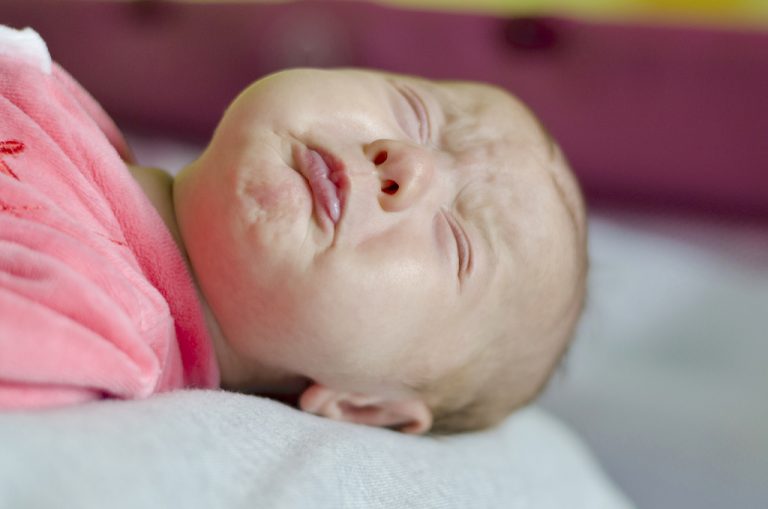
A child with a high fever may suffer from convulsions or seizures, which while scary to witness, are generally harmless. The child’s arms and legs will jerk involuntarily, their eyes may roll backwards, and their teeth may clench. Known as simple febrile fits, they can occur in children up to six years old. Each fit may last anywhere from one to 15 minutes. Try not to panic and don’t attempt to put any objects (spoon or finger) into their mouth. Instead, place the child on their side on a flat surface and wait for the fit to subside. Try to bring the fever down by sponging or with Paracetamol once the child is no longer drowsy.
Go to the A&E if febrile fits last longer than 15 minutes, if the child remains unusually drowsy or has mobility problems after the episode.
(See also: What is Kawasaki Disease?)
5. Acute Skin Conditions
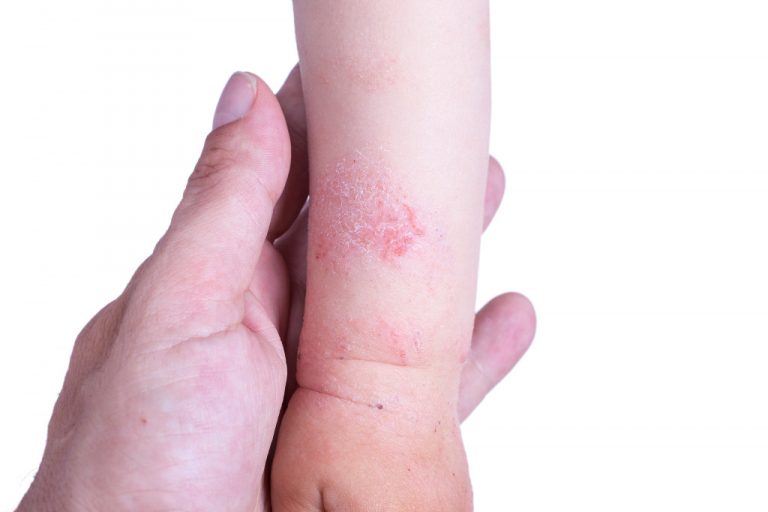
Executive Julia Chan, 33, relates how she decided to take her then seven-month-old boy to the KKH A&E immediately after picking him up from the nanny’s at about 10pm. “His nappy rash had worsened to where even his penis was raw and inflamed. She just sprinkled some powder and didn’t inform me about it earlier.” While it wasn’t a true emergency, the doctors said it was important to catch the infection early, especially given how young he was. They discharged him a few hours later.
Most skin conditions such as diaper rash or an eczema flare-up don’t usually constitute emergencies. However, some rashes may be a sign of something more severe, such as an acute allergic reaction to medication, and may need urgent medical attention. Rashes are also a common symptom of infectious viral diseases endemic to Singapore, such as dengue fever and HFMD (hand, foot and mouth disease).
HFMD is a highly infectious illness caused by intestinal viruses. Kids, especially under the age of five, are most susceptible. Symptoms include fever, sore throat, diarrhoea and vomiting, rash or small blisters on the palms of hands, soles of feet or buttocks, and ulcers on the inside of the mouth or sides of the tongue. Most cases of HFMD are mild, self-limiting and do not warrant a visit to the A&E. If your child is alert, visit your GP to confirm the diagnosis and observe the mandatory 10-day quarantine at home.
Go to the A&E if the rash erupted following a new medication, if the child is unable to eat, drink or urinate, has persistent vomiting, is excessively lethargic or drowsy, shows signs of dehydration.
(See also: Understanding Eczema in Babies & How to Deal with It)
6. Various Childhood Injuries
“We also visited the A&E in Chicago when Elliott was just three months old,” recalls Monica. “I took my eyes off him for just a second during a diaper change and he rolled off the (very high) bed.” Luckily, there was no lasting damage from the impact to his head.
It’s quite common for children to fall and hurt themselves, whether at home or while playing outdoors. While most can be brushed off with a kiss, some can have more dire consequences. Every year, about 4,700 to 5,500 children show up to the KKH A&E with head injuries. Younger children and babies are more predisposed to serious head traumas, and any injury to the head should be taken seriously. The likelihood of a severe outcome also increases with the height of the fall.
Other common childhood injuries seen at the A&E departments include or are caused by:
- Bone fractures
- Burns and scalds
- Accidental poisoning
- Accidental drowning
- Bleeding and open wounds
- Eye, ear and nose injuries
- Swallowed or inhaled objects
Go to the A&E if the child is below two years old, injuries are significant and/or result in vomiting, drowsiness, lethargy, unusual subdued behaviour or persistent irritability.
(See also: Comparing Children’s Hospitalisation Costs in Singapore – We Do the Homework for You)
Note: Use the A&E Wisely

Dr Kao Pao Tang, Head & Senior Consultant, Children’s Emergency, National University Hospital (NUH), would like to remind parents that all A&E departments have limited resources. “It would be really helpful if parents could make the effort to consult their GPs or 24-hour clinics first. Even if they are prepared to wait, overcrowding at an A&E has been shown to decrease the level of care delivered to those who need them most.”
“In fact,” continues Dr Kao, “only 11 to 14 per cent of visits by children to the A&E at NUH lead to hospitalisation.”
So, parents, take your children to the A&E only when it’s a real emergency. You’d be helping to save lives by freeing up A&E staff to attend to critical cases. Besides, if your child has a non-emergency condition, you’d be subjecting them to hours in a hospital waiting room – a hotbed of germs – unnecessarily. Instead, consider visiting a 24-hour GP clinic, where they’ll probably get treated sooner anyway.
All content from this article, including images, cannot be reproduced without credits or written permission from SingaporeMotherhood.
Follow us on Facebook, Instagram, and Telegram for the latest article and promotion updates.





