SingaporeMotherhood | Baby & Toddler
April 2018
Caring for your Child’s Skin and Managing Eczema

The skin is the largest organ in the body. Improper care of the skin results in unsightly rashes, and in serious cases, severe skin infections. Below is a discussion on one of the most common childhood skin problems.
Damien (not his real name) is a four-year-old boy who has been suffering from atopic dermatitis (AD) or eczema since birth. He has frequent skin flare-ups, which cause itchiness and discomfort. Recently, these flares have been lasting longer than usual and he has not been able to tolerate the itch well.
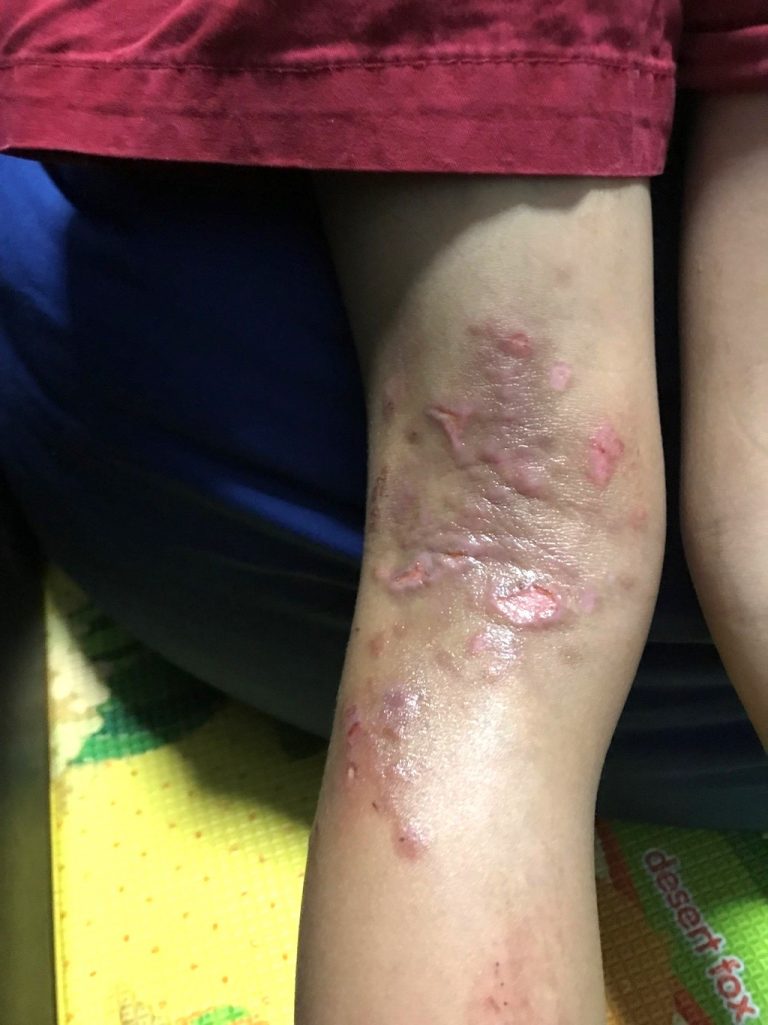
The last time I saw him, he was thin, tired, and uncomfortable. His whole family looked sleep-deprived. He could not stop scratching his skin, and at times he would let out wails of frustration. Damien’s skin was dry and scaly and he had trails of blood along broken skin, where his fingernails had clawed. His skin’s traumatic landscape included patchy areas of discharge and foul-smelling crusts caused by secondary bacterial infection.
But there was no relief in sight. His parents refused the use of topical steroids to treat him as they believed that steroids were harmful. His condition did not improve and he was discharged against advice.
A Rash Start
Rashes that are clearly visible on your child’s skin are usually a source of distress. Some rashes need early medical attention to prevent complications, for example, hemangiomas (growths of blood vessels). However, most rashes are benign and can resolve over time. Neonatal acne is an example of this. Other common skin conditions in children include birthmarks such as Mongolian spots.
Atopic Dermatitis (AD) is a very common recurrent skin condition in childhood. It can present at a very young age — even in newborns, in fact! Babies may have rashes on the scalp and cheeks, and these can extend to the neck and skin folds of the elbows and knees. Common triggers include sweating, changes in climate, viral illnesses, stress, insect bites, and environmental factors such as house dust mites.
What causes AD?
The causes of AD are multifactorial. There may be a personal or family history of atopy (tendency to develop classic allergic disease such as allergic rhinitis, eczema, asthma or allergic conjunctivitis). However, AD can also be a result of a combination of environmental and genetic factors. Gene mutations may result in dry skin which increases exposure to environmental antigens. This results in an immune inflammatory response which causes red and itchy skin. The more you scratch, the itchier it gets (what we know as the “itch-scratch cycle”).
Complications can also arise from this. They include viral or bacterial infections of the skin from scratching, thickening of the skin, and a child’s failure to thrive due to the uncontrolled disease. Severe cases may be associated with food allergies. However it is not routine to hunt for allergies with blood tests or skin prick tests unless there is a history of incidents that leads the doctor to believe that these are necessary.
Treating AD for Better Skin
The frequent use of moisturisers can help prevent eczema or atopic dermatitis (AD). It is crucial to preserve your child’s skin integrity as much as possible to prevent flares. Breastfeeding has been reported to reduce the risk of AD in high-risk infants (who have family history of atopy). Although there is no cure, the good news is that AD can be controlled. There are three ways to do that:
1. Moisturise, moisturise, moisturise. To stop the itch and treat AD, frequent use of moisturisers is necessary to hydrate the skin barrier. There is no one best moisturiser; as long as it works for the child, is affordable and the child can tolerate the sensation of the application, use it.
2. Use topical steroids. Topical steroids reduce the itch and quell skin inflammation. Steroids are naturally occurring hormones in the body and abuse of steroids can result in negative side effects. However, with proper supervision from a doctor, the use of steroids in AD is safe. Furthermore, there are different strengths of steroid creams. It is best to verify with your child’s doctor if you have queries about steroid use for your child, instead of reading websites on the Internet. This is because some websites may contain false information. The extreme irrational fear of Damien’s parents resulted in unnecessary suffering of their child. Topical steroids will usually be stopped when the skin flares resolve. Intermittent use of topical steroids does not result in side effects, dependence, or addiction.
3. Trigger avoidance. This is to reduce the frequency of flares. Environmental advice includes avoiding cigarette smoke, house dust mite control measures like regular cleaning of the household, including mattresses and bedding and soft toys, and avoiding harsh soaps for bathing.
Living well with AD
Although there is no definitive cure for AD, proper early control for the flares will enable the child to sleep well and lead a normal quality of life. When there are no flares, the child can take part in outdoor activities such as swimming as long as it is not between 10 am and 4 pm (when the UV rays are strong). Of course, you need to slather sun protection cream on any exposed skin. Wth proper treatment, many children (though not all) have seen good control of AD over time. Hence parents should not give up, but rather, persist with the treatment for their child.
To learn more about Raffles Children Centre or make an appointment with a paediatrician, visit: https://www.rafflesmedicalgroup.com/specialist-centres/services-by-centre/children
Dr Chong Jin Ho is a paediatrician who was previously an Adjunct Assistant Professor at the Duke-NUS Graduate Medical School, an Adjunct Instructor in the Department of Paediatrics, Yong Loo Lin School of Medicine and a clinical teacher in Lee Kong Chian School of Medicine. Dr Chong has a special interest in paediatric dermatology, which includes conditions such as atopic dermatitis (eczema), urticaria and skin infections.
Stay connected with Raffles Medical Group (@rafflesmedgrp) on Facebook, Twitter and Instagram.
This is a sponsored post.
Header image: Source
Featured image: Omar Lopez on Unsplash
All content from this article, including images, cannot be reproduced without credits or written permission from SingaporeMotherhood.
Follow us on Facebook, Instagram, Telegram, and TikTok for the latest article and promotion updates.