SingaporeMotherhood | Baby & Toddler
December 2014
Using Epidural for Normal Delivery
As a first-time mother, I spent 16 hours in labor. Going in and out of a pain I had never experienced before, I remember being told to curl up on my side “like a prawn” and not to move a muscle. The nurse held me still while a young doctor injected something into my spine. The relief that came soon after made me wonder why I hadn’t asked for it earlier.
As Cynthia Choo, 38, mother of one, describes, “Epidural is a God’s gift to ease the pain”.
Indeed. At the KK Women’s and Children’s Hospital, where as many as 35 children are born each day, about 5,000 epidurals are administered each year when mothers in labour ask for them. That is slightly over a third of all births there in a year. Private hospitals in Singapore offer epidural as part of maternity packages.
[banner][/banner]
Epidural has been used for women in labor since 1942. As with any medical procedure that laymen may not have intimate knowledge of, there are myths and misconceptions about it.
You may have heard, for instance, that it can negatively affect your health, or that it will increase the need for a C-section. Some even say that it prolongs the labour process. The truth? Different women react differently to the drug, and many misconceptions are just that – misconceptions. (Dr Eileen Lew, Head and Senior Consultant at the Department of Women’s Anaesthesia, KK Women’s and Children’s Hospital (KKH), demystifies them here)
You may even have heard that there is a ‘window of opportunity’ when it comes to epidural administration. That asking for epidural before or after this golden period is futile as it will be denied. But now, there is new research that clarifies when epidural should be given.
A team of obstetric anaesthesiology specialists from the KK Women’s and Children’s Hospital, Duke-NUS Graduate Medical School, Singapore Clinical Research Institute, and the NUS Yong Loo Lin School of Medicine in Singapore reviewed studies that had taken place between 1994 and 2012 to find out whether the timing of the epidural made a difference to childbirth outcomes. The report produced by The Cochrane Library can be viewed here.
This review, which studied 15,752 first-time-mothers over 18 years, concluded that the best time for epidural is — when you ask for it.
Experts from KK Women’s and Children’s Hospital (KKH) advocate this fact-based wisdom.
But first, more on epidural itself.
What is Epidural?
According to Health Promotion Board (HPB) Singapore, there are four kinds of pain relief available for pregnant women during labour:
1) Entonox (also known the laughing gas), which you breathe in through a mask.
2) Transcutaneous Electrical Nerve Stimulation (TENS) sets, which are battery-operated electrode pads taped to your back to stimulate the production of your natural pain-relieving hormones.
3) Pethidine, which is a drug similar to morphine injected into the thigh or buttock.
4) Epidural Analgesia, which is a local anaesthetic injected into the spine.
Obstetricians tell us mothers-to-be that epidural is regional anaesthesia or analgesia (pain relief) that diminishes pain in selected areas.
Dr Sng says that “in KKH, epidural analgesia (EA) is the preferred choice of pain relief during labour for first-time mothers. This is the gold standard when it comes to being able to provide the good pain relief with minimal or no sedation to the mother.”
Dr Lew explains, “Local anaesthetic drugs are injected into the epidural space, the outermost part of the spinal canal. The combined spinal-epidural analgesia (CSEA) differs from EA in that an initial dose of the drug is injected into the spinal space, which is also within the spinal canal. This results in faster pain relief. The choice of EA or CSEA is usually left to the anaesthesiologist, as dictated by the stage and progress of labour”.
While EA may take up to 20 minutes to work, CSEA relieves pain within five minutes.
The Pros and Cons of Epidural
Aside from pain relief, both EA and CSEA can help prevent blood pressure from reaching critically high levels during labour, in women who suffer from pregnancy-induced hypertension, Dr Lew explains.
She adds that epidural not only provides safe, consistent, and reliable pain relief during labour, it also enables the baby to have better blood flow during and between contractions. It also reduces many stress-related effects to the mother, protecting those with high blood pressure, pre-eclampsia, heart problems, or diabetes.
Of course, there could be side-effects. Some women get the shivers, feel itchy, nauseous, feverish, and experience muscle weakness and headaches. These usually pass after a while. It is very rare to hear of serious complications from this procedure.
Your legs would feel rubbery. But you would still feel your lower body by 20 percent, because you should still be able to push when it is time for the baby to come out.
The review found that while epidural does not affect the length of time spent during the pushing stage, it may and may not affect the time to reach full cervical dilation. Giving epidural early also does not affect the likelihood of needed an assisted birth involving forceps or suction.
When to Ask for Epidural?
In the Cochrane Library report, lead researcher Dr Sng confirms that “the right time to give the epidural is when the woman requests pain relief”. The Deputy Head and Senior Consultant of the Department of Women’s Anaesthesia, KK Women’s and Children’s Hospital (KKH), Singapore explains: “If they request an epidural early during their labour, the evidence we have does not provide a compelling reason why this should be refused.”
At the very least, the decision rests on the labouring mother’s pain threshold. As Cynthia shares, “My endurance level is low. I charged into the hospital at 8.30am. At 11am I decided to have my epidural.” Do note that it can take up to 30 minutes for the anaesthesiologist to arrive.
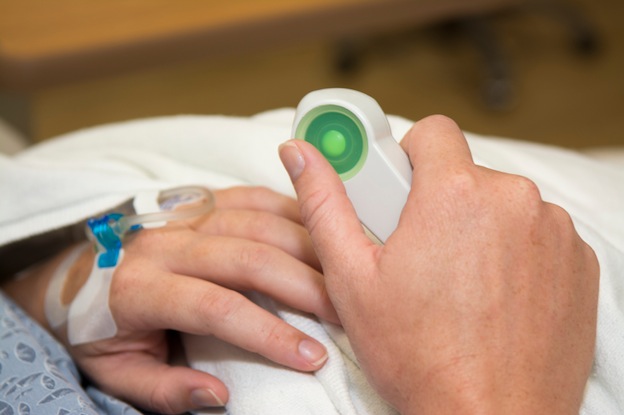
At KKH, besides EA and CSEA, a mother-to-be can choose to have patient-controlled epidural analgesia (PCEA). Although this has been used in clinical practice for over 25 years, it is not commonly known. The PCEA is a pre-programmed device which enables the mother to self-administer additional pain relieving medications into the epidural space by pressing onto a patient demand control button.
This allows mothers to individualise their own pain relief, based on their need. Because she has better control over her own pain, the mother-to-be may end up consuming less of the drug. And that would only be beneficial for both mother and child, wouldn’t it?
All content from this article, including images, cannot be reproduced without credits or written permission from SingaporeMotherhood.
Follow us on Facebook, Instagram, Telegram, and TikTok for the latest article and promotion updates.





