Angelica Cheng
Active Member
Many fertility clinic websites claim that PGS can improve IVF success for older women and patients with multiple IVF failures or recurrent miscarriages. However, there has recently been increasing contradictory information from different sources, which dispute the beneficial claims of PGS in IVF treatment.
Here is a summary of new scientific evidence that dispute the beneficial effects of PGS / PGT-A in IVF treatment:
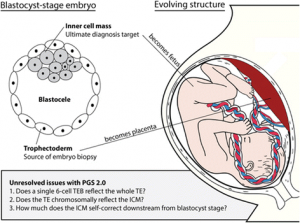
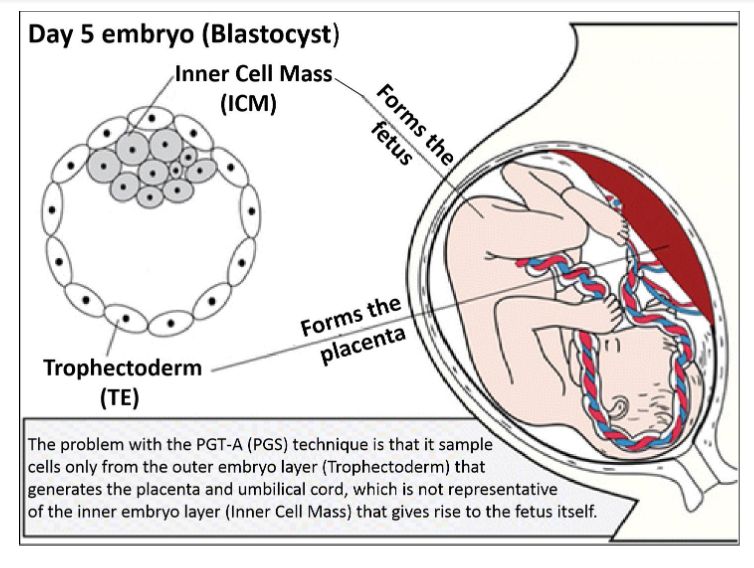
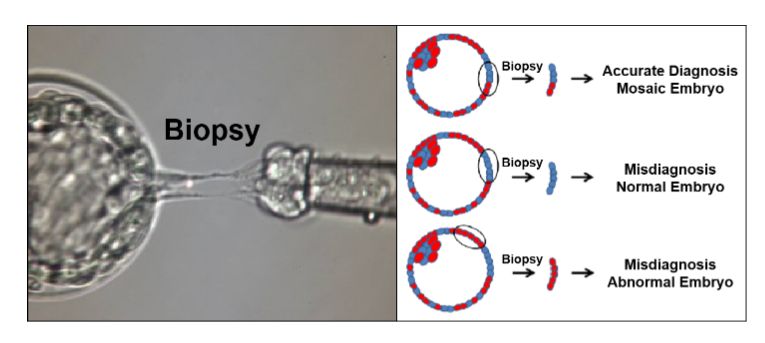
1) The biopsy procedure of PGS involve extracting and sampling cells from the outer embryo layer (Trophectoderm or TE) that gives rise to the placenta. This is not representative of the inner embryo layer (Inner Cell Mass, ICM) that goes on to form the actual embryo proper, which gives rise to the baby.
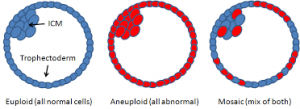
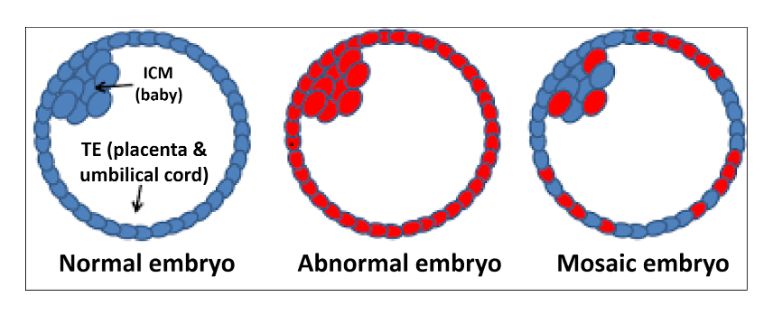
2) Mosaic embryos, which are embryos with a mixture of genetically normal (euploid) and abnormal cells (aneuploid) occur quite frequently and commonly among woman undergoing IVF (17% to 48%, please see link below). PGS often leads to the misdiagnosis and discarding of mosaic embryos, which have been shown to be capable of giving rise to a normal and healthy baby.

 www.fertilityiq.com
www.fertilityiq.com

 www.coopergenomics.com
www.coopergenomics.com
3) There is scientific evidence that Mosaic embryos are able to “self-correct”, which increases the chances of a normal birth. This “self-correction” mechanism involve pushing out the genetically abnormal (aneuploid) cells into the outer embryo layer (TE), which gives rise to the placenta.
 www.focusonreproduction.eu
www.focusonreproduction.eu

4) Older women with low ovarian reserves have much fewer embryos during IVF. Therefore excluding or discarding of mosaic embryos that can potentially give rise to a normal baby, would in fact substantially reduce their chances of IVF success. Some older women may have no embryos left to transfer after PGS.
5) The PGS biopsy procedure of extracting cells from the embryo can potentially harm the embryo, and impair it’s development. Experts have pointed out that studies claiming no ill effects to embryos are often based on PGS of excellent-quality, healthy, robust embryos rather than more “delicate” embryos that might suffer more. If you have just one or two embryos, you might decide it is not worth the risk.

 www.cnyfertility.com
www.cnyfertility.com
Here is a summary of new scientific evidence that dispute the beneficial effects of PGS / PGT-A in IVF treatment:
1) The biopsy procedure of PGS involve extracting and sampling cells from the outer embryo layer (Trophectoderm or TE) that gives rise to the placenta. This is not representative of the inner embryo layer (Inner Cell Mass, ICM) that goes on to form the actual embryo proper, which gives rise to the baby.
2) Mosaic embryos, which are embryos with a mixture of genetically normal (euploid) and abnormal cells (aneuploid) occur quite frequently and commonly among woman undergoing IVF (17% to 48%, please see link below). PGS often leads to the misdiagnosis and discarding of mosaic embryos, which have been shown to be capable of giving rise to a normal and healthy baby.

What Is Mosaicism & Why Should I Care?
Embryos that are mosaic have a combination of normal and abnormal cells and lead to a live birth in 20%–30% of transfers. Rates of "mosaicism" vary based upon the definition but are often believed to represent 1 in 5 embryos.

New Study Bolsters View That Mosaic Embryos From IVF Can Develop Into Healthy Babies
This article originally was published on GenomeWeb on July 14th, 2017 by Julia Karow. NEW YORK (GenomeWeb) – To increase the ...
3) There is scientific evidence that Mosaic embryos are able to “self-correct”, which increases the chances of a normal birth. This “self-correction” mechanism involve pushing out the genetically abnormal (aneuploid) cells into the outer embryo layer (TE), which gives rise to the placenta.

Self-correction and the potential of mosaic embryos to implant
The transfer of chromosomally 'abnormal' embryos can still result in pregnancy in IVF: New study helps resolve controversy over self-correcting 'mosaic' embryos
IVF embryos whose cells have mixed chromosomal profiles -- one normal, another abnormal -- still have the potential to implant in the uterus and become a healthy pregnancy, according to a new study.
www.sciencedaily.com
4) Older women with low ovarian reserves have much fewer embryos during IVF. Therefore excluding or discarding of mosaic embryos that can potentially give rise to a normal baby, would in fact substantially reduce their chances of IVF success. Some older women may have no embryos left to transfer after PGS.
5) The PGS biopsy procedure of extracting cells from the embryo can potentially harm the embryo, and impair it’s development. Experts have pointed out that studies claiming no ill effects to embryos are often based on PGS of excellent-quality, healthy, robust embryos rather than more “delicate” embryos that might suffer more. If you have just one or two embryos, you might decide it is not worth the risk.

PGS Testing Risks
PGS testing (aka PGT-A) is not without risk. It's a common selection tool for choosing the best embryo to transfer during In Vitro Fertilization (IVF). Using a laser, a small biopsy of the embryo is taken and the DNA inside the sample is analyzed. Does this biopsy harm the embryo? Does PGS...
Last edited: