SingaporeMotherhood | Pregnancy
October 2012
The ART of Making Babies
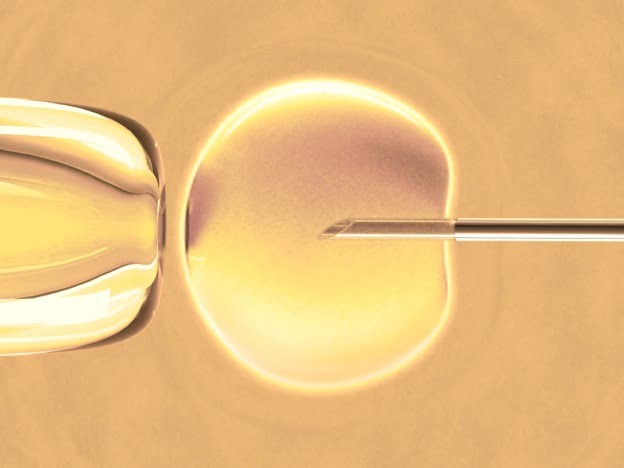
On 25 July 1978, Louise Joy Brown, better known as the world’s first test-tube baby, was born. She was the result of an experimental procedure called in vitro fertilisation (IVF), where doctors joined her mother’s egg and her father’s sperm in a glass dish in a laboratory. This was the very first time conception had taken place outside a woman’s body.
[banner][/banner]
Today’s Technologies
With medical technology having since advanced by leaps and bounds, couples facing fertility problems can now take advantage of not just IVF, but several assisted conception treatments tailored to each unique condition.
These procedures come under the umbrella term of Assisted Reproduction Technology – ART for short – and are usually paired with more conventional therapies such as fertility drugs to increase success rates.
Worldwide, almost one out of every three cycles of ART results in the birth of a baby for women under 35. In spite of this, many doctors usually recommend ART as a last resort, rather than a default go-to. They prefer to assist couples in exploring other assisted conception treatments first, as ART procedures are invasive, stressful, and expensive.
Janis Heng, 36, went through three rounds of ART between December 2010 and March 2012 – two IVF procedures with one IVM (in vitro maturation) treatment in between.
The procedures were not easy to endure. “I really dreaded having needles poking into my tummy. Because of too many follicles in my ovaries, my tummy became bloated and this made poking in the needles even more difficult,” the business executive shares.
But the hardest part was the two-week wait for results. “The emotional highs and lows were tough and took a while to get over,” Janis recalls.
Success Rates
Much depends on the age of the woman. Women aged below 35 have up to 40 per cent chance of conception with IVF. For those above 40 years, success rates fall to around 10 per cent.
Dr Stephen Chew, Senior Consultant at the National University Hospital (NUH) Women’s Centre, observes: “We are seeing more patients above 35 years old seeking ART services; this has increased by approximately 10 per cent in the last 10 years. We are also seeing more women seeking IVF in particular. In fact, there has been a six per cent increase in initiated cycles the last three years.”
Dr Chew continues, “Although this is a trend as more women marry older and delay child-bearing, this does hamper our ability to help our patients achieve their desired pregnancy, as IVF results are very much tied to the age of the woman. A woman’s ‘biological clock’ and eggs age with time; this will impact her chances of pregnancy.”
For those trying to conceive, Dr Chew advises, “If you do not fall pregnant after one year of trying, start seeking help. Fertility treatment should be started early to avoid disappointment and for a better success rate. Similarly, undue delays can impact your ultimate chances of a successful pregnancy.”
Here is a general guide to the various techniques used in ART and other assisted conception treatment options.
Fertility Drugs
A woman is treated with fertility drugs to regulate her reproductive hormones and trigger the release of eggs during her ovulation cycle. While this is typically the first line of action because it is the least invasive, fertility drugs are also used in conjunction with most other assisted conception treatments.
Best for
Women exploring fertility treatment for the first time .
Contraindications
The drugs can cause side effects such as headaches, cramping, bloating and Ovarian Hyperstimulation Syndrome (OHSS), and increase the odds of multiple births.
Success rate
20% – 60%. Most women use fertility drugs for three to six months. If they do not conceive with this, they will go on to explore other treatments.
Intrauterine insemination (IUI)
The most commonly used method of artificial insemination. Around the time of her ovulation, a concentrated dose of her partner’s sperm is injected into woman’s uterus using a fine catheter. This places the sperm close to the egg and raises the chance of fertilisation. Fertility drugs may be used before the procedure.
Best for
Women with unreceptive cervical mucus; men with poor sperm motility.
Contraindications
Cramping for up to two days.
Success rate
5% – 25%
In vitro fertilisation (IVF)
The most commonly used ART option, this also has the highest success rates. After undergoing ovarian stimulation, a woman’s eggs are harvested from her ovaries and combined in a laboratory with her partner’s (or donor) sperm. Once fertilisation takes place, the resulting embryos are allowed to develop for a few days before being placed in the woman’s uterus.
Best for
Women with blocked or damaged fallopian tubes, endometriosis, ovulatory or immunological problems, as well as male factors .
Contraindications
Highly invasive, the process involves multiple injections of fertility drugs, blood tests, repeated scans, a surgical procedure and all their possible side effects .
Success rate
28% – 35%
Intracytoplasmic sperm injection (ICSI)
Using a microscopic needle, a woman’s egg is injected with her partner’s (or donor) sperm in a laboratory. Once fertilisation takes place, the embryo is allowed to develop for a few days before being placed in the woman’s uterus.
Best for
Couples who have failed to achieve fertilisation via IVF; men with abnormal sperm parameters.
Contraindications
In addition to the IVF contraindications, sperm may need to be drawn with a microscopic needle or surgical biopsy.
Success rate
About 35%
In vitro maturation (IVM)
A new, less invasive and less costly variation of IVF where a woman’s immature eggs are harvested from unstimulated or minimally stimulated ovaries. They are matured in the laboratory for one to two days before IVF or ICSI is performed.
Best for
Women who are at high risk for OHSS; those who had immature eggs salvaged from IVF/ICSI previously; those below 35 with antral follicle count of 10 or more.
Contraindications
As this is a relatively new procedure, long term safety records are lacking .
Success rate
28% – 35%
Gamete intrafallopian transfer (GIFT)
A woman’s eggs are combined with her partner’s (or donor) sperm in a laboratory, then surgically placed in the woman’s fallopian tubes via laparoscopy. The aim is for fertilisation to take place within her body and for the embryo to implant naturally.
Best for
Couples with unexplained infertility; women with minimal endometriosis .
Contraindications
Longer recovery time and lower success rates than IVF, but with the same possible side effects.
Success rate
25%-30%
Zygote intrafallopian transfer (ZIFT)
Similar to GIFT, a woman’s eggs are combined with her partner’s (or donor) sperm in a laboratory, then surgically placed in her fallopian tubes via laparoscopy. However, with ZIFT, the doctor will wait till fertilisation occurs in the laboratory before proceeding with the procedure.
Best for
Women who are keen to try GIFT, but have a lower chance of fertilisation; women over 40 years of age.
Contraindications
Longer recovery and laboratory waiting time and lower success rates than IVF, but with the same possible side effects .
Success rate
25% – 30%
Donor egg/embryo
A variation of the other ART options where a woman’s eggs are found to be unable to result in conception. Her partner’s (or donor) sperm is mixed in a laboratory with a donated egg, with the resulting embryo implanted in the woman’s uterus via IVF techniques. This same procedure can be done with a donated embryo.
Best for
Women who are unable to produce eggs; women at risk of passing on an inherited disease. For donated embryos, couples with complete infertility; couples at risk of passing on an inherited disease.
Contraindications
Choosing the egg/embryo donor can be a long process; a possible sense of loss at not having a baby with complete genetic ties .
Success rate
About 43%
Surrogacy
A variation of the other ART options where a woman’s body is found to be unsuitable to carry the baby to full-term for various reasons. In this case, the embryo is implanted in the uterus of another woman who acts as a gestational carrier and gives the baby to the couple after birth.
Best for
Women with a damaged or non-existent uterus; women for whom a pregnancy would be life-threatening due to medical problems .
Contraindications
Having little control over the pregnancy, the carrier’s diet and lifestyle, etc .
Success rate
Currently unavailable.
Medisave may be used to offset the costs of certain procedures. Some procedures may be co-funded by the government. See the Ministry of Health website for details.
All content from this article, including images, cannot be reproduced without credits or written permission from SingaporeMotherhood.
Follow us on Facebook, Instagram, and Telegram for the latest article and promotion updates.






