SingaporeMotherhood | Pregnancy
December 2013
Road to a Successful C-Section

Wong Lina, 37, who manages a travel agency, is the mother of three children aged 12, 10 and 5. She delivered all her babies through C-section. For the first one, she had anticipated normal birth, but had vaginal herpes, which was detected late in the pregnancy. Since she did not want to risk infecting her baby during labour, she listened to her obstetrician and opted for a C-section.
For the second one, she was again hoping to deliver normally. But when her cervix stopped dilating stopped at four centimetres and she was feeling too weak to go on, her husband talked her into going under the knife. It turned out the baby was bigger than expected. After two C-sections, she simply decided on a C-section for her third baby. Delivering her babies via C-sections was not a problem for Lina. her priority was the health and safety of her babies, not the way they were born.
[banner][/banner]
Caesarean sections have been around for over 500 years. But with increased awareness of the benefits of a natural birth for both mother and baby, C-sections, as Caesarean surgeries are commonly known as, have somewhat of a stigma attached to them. “Women are over four times more likely to have a caesarean birth now than they were thirty years ago and eight times more likely than they were fifty years ago,” say Helen Churchill and Wendy Savage, authors of How to Avoid an Unnecessary Caesarean: A Handbook for Women Who Want a Natural Birth.
A 2008 study by the World Health Organisation (WHO) listed the global average for c-sections then as 15 per cent. In Singapore, there is a general consensus among obstetricians to aim for normal delivery at all times. If the mother-to-be is healthy and the baby is normal, it is not advisable to plan for a C-section just so the baby can be born on or before a certain date. Having said that, according to the National University Hospital (NUH)’s Women’s Centre, about 26 to 27 per cent of the births there over the last five years are Caesarean births. The number has remained stagnant, but that means about one in every four women goes under the knife to deliver her baby.
According to Dr. Fong Kah Leng, an obstetrician and gynaecologist in private practice, the most common reason (35 %) for this procedure is that the mother has had a previous C-section. This is because previous C-section scars tend to be weak and may tear open during a normal vaginal delivery. The next reason (30 %) is due to a difficult labor due to non-progression. This could be caused by abnormalities in the mother’s birth canal or in the position of the foetus.
Another common factor is foetal distress, a condition where the foetus is not getting enough oxygen. During the course of labour or even before the onset of labour, if a baby at or near full term is found to have a slow or irregular heart rate, this is a signal of distress for the baby. The baby may also send SOS signals by passing meconium or faeces.
In addition to these, the mother’s health may make delivery by C-section the safer choice, especially in cases of maternal diabetes, hypertension, vaginal herpes, multiple pregnancy, Rh blood incompatibility, pre-eclampsia and HIV infection. Lisa Ho, 39, delivered her daughter Gabriella via C-section at 36 weeks of gestation. The SAHM, who used to work in the IT industry, was hoping for a natural birth, but found that she had placenta previa (low-lying placenta) in ger 26th week of pregnancy. By the 36th week it was confirmed that the baby was not growing as well as it should, and her obgyn suggested a C-section.
The Disadvantages of a C-Section
Because a C-section is a surgical procedure, it carries more risk to both the mother and the baby. The maternal mortality rate is less than 0.02 %, but that is four times the maternal death rate associated with vaginal delivery.
The mother is at risk for increased bleeding because a C-section may result in twice the blood loss of a vaginal delivery. Although complications occur in less than 10 % of cases, the mother may develop infection at the incision, the urinary tract, or the tissue lining the uterus (endometritis). Less commonly, she may receive injury to the surrounding organs, such as the bladder and bowel. And when a general anesthesia is used, she may experience complications from the anesthesia.
Very rarely but not impossibly, a woman may develop a wound hematoma at the incision site or other blood clots leading to pelvic thrombophlebitis (inflammation of the major vein running from the pelvis into the leg), or a pulmonary embolus which is a blood clot lodging in the lung.
What Happens Before, During, and After C-Section
Caesareans can be done in both private and public hospitals in Singapore. Your Medisave can cover a part of it. When a C-section becomes necessary, the mother is prepped for surgery. Ideally, she should have fasted for about four hours. A catheter is inserted into her bladder and an intravenous (IV) line is inserted into her arm. The nurse would attach leads to monitor the mother’s heart rate, rhythm, and blood pressure.
In the operating room, the mother is given anesthesia – usually a regional anesthesia by epidural or spinal – making her numb from below her breasts to her toes. In some cases, a general anesthesia will be administered. Surgical drapes are placed over the body to block the direct view of the procedure.
The abdomen is washed with an anti-bacterial solution and a portion of the pubic hair may be shaved. It is generally five minutes from the time of the initial incision until the baby is born. From birth through suturing is about 30 to 40 minutes. The entire surgical procedure may be performed in less than one hour.
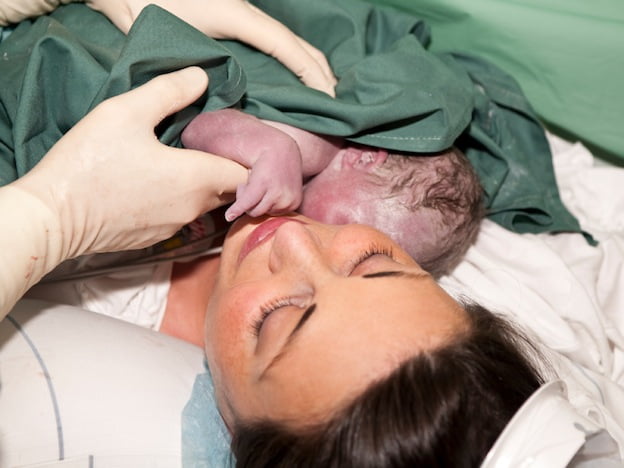
Ms Ginny Phang, a doula from Four Trimesters, encourages mums to start bonding with their newborns as soon as possible. If you have opted for an epidural instead of general anaesthetic, you will be conscious and able to do so. Pre-delivery, arrange with your doctor to have your baby be laid on your bare chest for a skin-to-skin contact within the first two hours of birth, while she is at her most alert. This contact benefits both mother and baby.
Recovery After a C-Section
The after-effects of a C-section vary, depending on the woman’s age, physical fitness, and overall health. Following this procedure, a woman commonly experiences gas pains, incision pain, and uterine contractions – which are also common in vaginal delivery. Her hospital stay may last between two and four days. Breastfeeding is encouraged, in a position that keeps the baby from resting on the mother’s incision.
A woman who undergoes a C-section requires both the care given to any new mother and the care given to any patient recovering from major surgery. She should be offered analgesia to manage her pain. These medications should not interfere with breastfeeding. She will be encouraged to get out of bed and move about eight to 24 hours after surgery to stimulate circulation – thus avoiding the formation of blood clots – and bowel movement. Climbing stairs should be limited to once a day, and anything heavier than the baby is too much for her to carry.
A mother generally multi-tasks, therefore she should delegate her tasks and arrange for help with the housework, meals, and care of other children. She should not feel guilty to nap as often as the baby naps, because she needs all the rest she can get to recover. Driving may resume after two weeks, but some doctors recommend waiting six weeks, which is the typical recovery period from major surgery.
Post-Caesarean Tips
- Pack loose fitting dresses in your hospital bag. Try not to wear anything confining around your waist for the first week at least.
- When getting up from bed, turn onto your side and get up sideways.
- Eat very soft food like strained porridge for the first 24 hours.
- Start to breastfeed right away, even though your milk supply may be delayed.
- You can resume sexual activity after four to six weeks.
- Wait until after three months (preferably after a year) for your next pregnancy.
Following the advice of her traditional mother, Mieke Elvira, who works in a securities company, wore a tummy wrap after her C-section. But she only wore it loosely during the first week. She also ate confinement meals – mostly chicken cooked in wine – after two weeks. She tried to avoid seafood and eat less salt throughout her confinement period as these may cause itching at the wound. To speed up the healing of the wound, she took ‘Pien Tze Huang’, a Chinese medicine popularly used to combat inflammation.
As the woman heals, she may gradually do appropriate exercises to regain abdominal tone. Full recovery may be seen in four to six weeks. Dr. Fong reminds us that women who undergo a C-section should be encouraged to share their feelings with others to prevent postpartum depression. Women should also be encouraged to seek professional help if negative emotions surface.
If you are expecting your first child, it would be beneficial to speak to other mums to get a wider perspective of what each kind of deliver option entails. You may change your mind after hearing about their experiences. You should also do your own research and speak to your obgyn about your choices.
All content from this article, including images, cannot be reproduced without credits or written permission from SingaporeMotherhood.
Follow us on Facebook, Instagram, and Telegram for the latest article and promotion updates.





